Schedule a Consultation
216-621-3000Schedule a Consultation
216-621-3000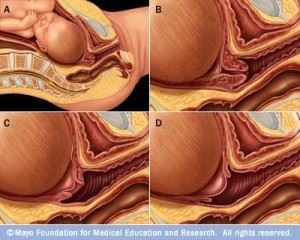
An important part of discovering whether doctors or nurses acted negligently during pregnancy, labor and delivery is understanding the stages of labor. The standard of care is based on what medical practitioners should do under any given set of circumstances. Those circumstances are important.
During the first stage of labor, the cervix opens (dilates) and thins out (effaces) to allow the baby to move into the birth canal. In figures A and B, the cervix is tightly closed. In figure C, the cervix is 60 percent effaced and 1 to 2 cm dilated. In figure D, the cervix is 90 percent effaced and 4 to 5 cm dilated. The cervix must be 100 percent effaced and 10 centimeters dilated before a vaginal delivery.
The first stage of labor begins with the beginning of labor and continues until the cervix is completely dilated and effaced. Dilation is the opening of the cervix (described in centimeters) and effacement is the thinning of the cervix (described as a percentage, from 0% to 100%). This stage averages about 10 to 12 hours for a mother having her first child, and 6 to 8 hours for mother who has had previous deliveries.
There are two phases in Stage 1: the latent phase and the active phase. The latent phase typically lasts from the beginning of labor until about 4 cm dilation. As the cervix opens, most women notice their “bloody show.” Many women can go about their daily routines during this period, as contractions are often not severe.
In the active phase, the cervix reaches a dilation of about 9 cm. The contractions are much stronger, closer together, and last longer. By the conclusion (sometimes called a third phase, the transitionphase), the cervix is completely dilated. Doctors and nurses should be watchful of the mother’s progress in terms of dilation and effacement. If insufficient progress is being made, the doctors should be particularly concerned about cephalopelvic disproportion, a condition where the baby could be too large to effectively pass through the birth canal.
Stage two proceeds from full dilation through to delivery. For women with no prior deliveries, this stage averages two hours (up to three if an epidural was used). For women with prior deliveries, this stage averages one hour (up to two if an epidural was used). If this stage lasts too long, doctors and nurses should be concerned about large babies (called fetal macrosomia), and a baby who is not in the proper position for delivery. Electronic fetal monitoring is particularly important to monitor whether the baby is receiving sufficient oxygen.
As the baby is delivered vaginally, the medical providers will be mindful of the problems associated with shoulder dystocia and an umbilical cord that is wrapped around the baby’s neck (called a nuchal cord). In some cases, it may be necessary to use forceps or vacuum for delivery. Of course, a cesarean section may be required, depending on the condition of the baby and the progress of labor.
The final stage of labor encompasses the period after delivery of the baby to the delivery of the placenta. The delivering health care provider, whether an obstetrician, family doctor or midwife, must ensure that the full placenta was delivered. If part of the placenta is retained in the mother’s body, it must be removed or else maternal infection or serious blood loss could set in.
Our birth injury lawyers are experienced in understanding all facets of the labor and delivery process, and we work closely with highly-credentialed doctors to prove our clients’ birth injury lawsuits. If you have questions about whether you are eligible for a medical malpractice lawsuit, contact us at 216-621-3000 or send us an online message.

