Schedule a Consultation
216-480-4620Schedule a Consultation
216-480-4620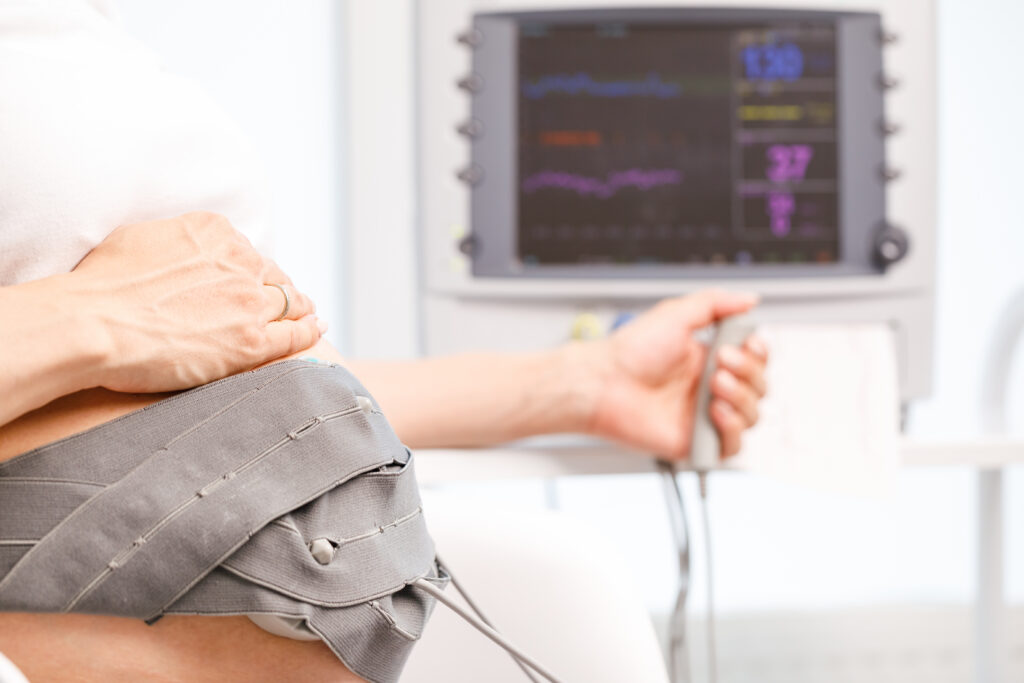
When a baby suffers a brain injury during labor and delivery, one of the first areas for concern is fetal monitoring. Continuous electronic fetal monitoring exists for a single purpose, to detect signs of hypoxia before irreversible neurological damage occurs. Understanding how these systems work and how providers are expected to respond is essential for families trying to make sense of what happened during delivery.
For nearly 50 years, The Becker Law Firm has represented Ohio families whose children have suffered birth injuries, including those caused by mismanaged labor and delayed responses to fetal distress. Our Cleveland birth injury lawyers work with medical experts who understand fetal monitoring standards, obstetrical decision-making, and the clinical benchmarks providers are expected to follow. If your child was diagnosed with HIE and you have questions about whether the care provided during labor met the appropriate standard, call our birth injury attorneys today at 216-480-4620.
In cases of hypoxic-ischemic encephalopathy (HIE), a condition caused by oxygen deprivation to the infant brain around the time of birth, a careful review of fetal heart rate tracings, emergency response timing, and umbilical cord blood gas results often forms the entire foundation of any legal analysis.
During labor, a fetus depends entirely on the placenta and umbilical cord for oxygen. When that supply is compromised, whether by cord compression, placental dysfunction, uterine hyperstimulation, or other causes, the fetal heart rate will often reflect the stress.
Continuous electronic fetal monitoring (EFM) allows providers to track these changes in real time. Patterns that deviate from normal baselines serve as warning signals that the fetus may not be tolerating labor well. The earlier those signals are recognized and acted upon, the greater the chance of preventing permanent neurological injury.
Obstetrical providers use two primary methods to monitor fetal heart rate during labor:
Both methods generate the electronic record known as a fetal heart rate tracing, sometimes called a cardiotocograph or CTG strip. These records can be used as evidence in any subsequent legal review with The Becker Law Firm.
The National Institute of Child Health and Human Development (NICHD) established a three-tier classification system for interpreting fetal heart rate tracings. This framework is widely adopted in obstetrical practice and sets the standard for provider conduct.
Category I tracings reflect normal fetal status. This includes a baseline heart rate between 110 and 160 beats per minute, moderate variability, the absence of late or variable decelerations, and the presence of accelerations.
A Category I tracing is typically reassuring and does not require immediate intervention beyond standard monitoring.
Category II tracings fall between normal and abnormal. This is not immediately alarming, but is entirely not reassuring either. This category encompasses a wide range of patterns that require heightened surveillance, clinical evaluation, and in many cases, intrauterine resuscitative measures.
The challenge with Category II tracings is that clinical judgment plays a significant role. Providers must assess the overall clinical picture, including the progress of labor, maternal condition, and any trends in the tracing over time.
When a Category II fetal monitoring tracing signals concerning patterns but providers fail to respond appropriately, this management lapse often becomes a key issue in birth injury litigation.
Category III tracings are abnormal and demand prompt action. This includes sinusoidal patterns and tracings with absent baseline variability accompanied by recurrent late decelerations, recurrent variable decelerations, or bradycardia.
A Category III tracing is a sign that the fetus is at significant risk.
Providers must act quickly, either through intrauterine resuscitation or expedited delivery, depending on the clinical circumstances. Failure to recognize a Category III pattern or delays in acting upon it can result in catastrophic and irreversible neurological injury.
At The Becker Law Firm, we help families hold hospitals accountable when delayed decisions during non-reassuring fetal heart rate tracings lead to birth injuries like HIE. Our medical malpractice attorneys are well-versed in handling these claims and securing the compensation your family needs to move forward.
When a non-reassuring fetal heart rate pattern develops, the obstetrical team's first response is typically to attempt intrauterine resuscitation before moving to operative delivery. Common measures include:
These measures are intended to improve fetal oxygenation and allow labor to continue safely.
When intrauterine resuscitation fails to resolve a non-reassuring or abnormal tracing, the standard of care typically requires expedited delivery. This may mean an operative vaginal delivery using forceps or vacuum, or an emergency cesarean section.
The decision requires quick clinical judgment that gives the baby the best chance of avoiding permanent injury.
When emergency C-section delays during fetal distress cause HIE or other birth injuries, The Becker Law Firm knows how to hold hospitals accountable for their actions or inactions during labor and delivery.
In an emergency cesarean section, the interval between the decision to operate and the first surgical incision is referred to as the decision-to-incision (DTI) time. Professional organizations, including the American College of Obstetricians and Gynecologists (ACOG), have issued guidance on acceptable DTI intervals.
When fetal distress is severe, prolonged delays in getting the baby delivered can result in additional oxygen deprivation and worsen neurological outcomes. In HIE litigation, the DTI interval is frequently scrutinized. Experts examine hospital records, nursing notes, anesthesia records, and operative reports to reconstruct the timeline and determine whether the care team responded with adequate urgency.
The medical record created during labor and delivery is often the primary source of evidence in HIE cases. Key records include:
Discrepancies between these records, or gaps in documentation at critical moments, can raise important questions about what happened and why.
HIE analysis requires a detail oriented attorney who understands how umbilical cord gases can create oxygen deprivation during labor. Our medical malpractice attorneys can leverage this knowledge to create a compelling case on your behalf.
Umbilical cord blood gases are drawn from the umbilical artery and vein at the time of delivery and provide objective data about the infant's oxygenation status at birth. The most important values are pH, which reflects the acidity of the blood, and base deficit, which measures the degree of metabolic acidosis.
A low pH combined with a significant base deficit is consistent with fetal acidemia, a condition that can result from oxygen deprivation during labor. These values help establish whether the infant experienced a hypoxic event and can help when determining the timing and severity for a legal claim.
HIE litigation often hinges on whether the newborn’s injury stemmed from an acute, preventable labor event or a prolonged pre-labor process. Cord gases, paired with fetal heart tracings, placental pathology, and newborn exam, enable experts to differentiate the potential causes. Acute intrapartum hypoxia ties more directly to provider actions, strengthening causation in legal claims.
When fetal monitoring and labor management are careless or delayed, preventable HIE injuries can become the basis for a malpractice claim against the delivery team. The personal injury team at The Becker Law Firm can help you understand if your child experienced a birth injury during labor and delivery. We aren’t afraid to take on hospitals and their staff to secure the compensation your family deserves.
Providers are trained to recognize and respond to questionable fetal heart rate patterns. When a Category III tracing is present and the medical team does not act with urgency, the consequences can be devastating. Expert witnesses in HIE cases review the tracing strip in detail, often minute by minute, to assess whether the patterns present should have prompted an earlier or more aggressive clinical response.
Persistent bradycardia, a sustained drop in fetal heart rate below 110 beats per minute, is one of the most urgent fetal heart rate findings in obstetrical care. When documentation shows that providers were aware of these findings and failed to respond in a timely manner, those facts can form the basis of a birth negligence claim.
It is important to acknowledge that not every infant who experiences HIE does so because of provider negligence. Birth is a complex physiological process, and some outcomes reflect events that were not foreseeable or preventable.
Hypoxic-ischemic encephalopathy can result from conditions such as placental abruption, uterine rupture, or severe umbilical cord prolapse, where even the most competent and attentive obstetrical team may be unable to prevent injury. A thorough expert review of the medical records is the only way to assess whether the care provided met the applicable standard of care and whether the outcome could reasonably have been different with different management.
The Becker Law Firm has secured landmark HIE-related case results, including a $10.1 million settlement for a boy with permanent brain injury from negligence and a $25.5 million settlement for a newborn who suffered oxygen deprivation due to protocol failures. This is one of the largest medical malpractice wins in Ohio’s history.
A thorough investigation of a potential HIE claim begins with a complete review of the labor and delivery record. Our legal team obtains and analyzes all relevant documentation, including:
At The Becker Law Firm, we work with board-certified obstetricians, maternal-fetal medicine specialists, neonatologists, and pediatric neurologists who review these records and provide expert opinions on the standard of care and causation. Their analysis is essential to building a credible and well-supported claim on behalf of your family.
Families navigating a child's HIE diagnosis face enormous challenges. The Becker Law Firm handles these cases with the seriousness and sensitivity they deserve. We are here to help you through every step of the process, including:
Ohio law sets specific time limits for filing birth injury claims. Families typically only have one year from discovering the injury to file a claim.
If your child was diagnosed with HIE and you have questions about whether the labor and delivery care was appropriate, contact our Cleveland birth injury attorneys today at 216-480-4620 to schedule your free, confidential consultation. There is no fee unless we recover compensation for your family.

